
“Controlled burn at Joseph W. Jones Ecological Research Center at Ichauway
in Newton, Ga. in 2016 Source: https://phil.cdc.gov/Details.aspx?pid=22804“
BIOAEROSOLS in WILDFIRE SMOKE
https://science.org/doi/10.1126/science.abe8116
https://asm.org/Articles/2021/April/The-Microbiology-of-Wildfires
The Microbiology of Wildfires
by Kanika Khanna / April 16, 2021
“One morning in September 2020, I, like many other residents of California and Oregon, woke up to an orange sky outside of my window. The eerie color and nature of the sky were due to the biggest wildfires that have ever engulfed California. While extensive work has been done on the effects of wildfires on terrestrial ecosystems, relatively few studies have focused on the effects of wildfires on soil microbiota or the microbial nature of the wildfires themselves. A wildfire can cause surface temperatures to reach above 1000°C, which is approximately the temperature of lava erupting from a Hawaiian volcano. These extreme temperatures, in addition to changing the physical properties and chemical structure of the soil, also adversely affect fungi and bacteria that inhabit its topmost layer. In general, survival favors microbial communities found in deeper soils, and bacteria have better heat tolerance than fungi.
In 2019, Whitman et al. investigated the effects of wildfire on microbial communities in the northwestern Canadian boreal forests and found that the community composition of burned area significantly differs from that of unburned areas, with increased abundances of bacterial species in the genera Massilia and Arthrobacter, and fungi in the genera Penicillium and Fusicladium. Mikita-Barbato et al. studied microbial community structure in organic horizon soils (the soil layer above the top layer of the soil with mostly organic matter, such as decomposing leaves, twigs, moss and lichens on the surface) of the New Jersey Pinelands over a period of 2 years post fire. They found that the composition of bacteria, fungi and archaea changed more dramatically during the first year and slowly during the second year, but still differed significantly from unburned soil. Another study analyzed the effects of different intensities of fire (low, moderate and high) on bacterial community composition in the topsoil (0-10 cm) and the sub-soil (10-20 cm) 6 months post fire. The authors observed several differences in bacterial communities inhabiting the topsoil and the sub-soil and these differences correlated with differences in pH, total nitrogen and ammonium nitrogen between the 2 soil types. Together, these findings suggest that the recovery of the physicochemical properties and microbial communities in soil may be very slow after a wildfire, forecasting long-term consequences for the soil ecosystem.

“Regenerating dry sclerophyll forest in Brisbane Water National Park, Australia 76 days post controlled burn conducted May 2013.” Source: flickr.com/photos/dougbeckers/9468779130
Another underexplored area of research is the microbiology of wildfires themselves. The aerosol nature of wildfire smoke can transport ash, dust and harmful chemicals over long distances. Extensive research has been done on the adverse effects of particulate matter in wildfire smoke on human cardiovascular and respiratory health. Recent evidence suggests that wildfire smoke can also aerosolize and transport living things, including bacteria, fungi and their metabolic products. This field of “pyroaeromicrobiology,” which lies at the intersection of fire ecology, atmospheric sciences and microbiology, has the potential to uncover the role of wildfires in spreading pathogenic and beneficial microbes in the ecosphere. Like the fire itself, the temperature of wildfire smoke can reach above the tolerances of many life forms. However, variability in the kind of fuels, availability of oxygen and other meteorological factors can create a wide array of biological niches that may favor different populations of microbes in space and time. There is evidence that microbes directly hitchhike on the particulate matter found in wildfire smoke. Pyrogenic carbon produced by wildfire can be a temporary substrate for aerosolized soil microbes, and the obscuring of ultraviolet radiation by particulate matter boosts the viability of bioaerosols.
Wildfires generate convective air currents that carry the hot fire straight up while cooling air descends to create a cyclical pattern heat column. Such dynamic movements further enhance the concentration of bioaerosols like fungal spores in the smoke. Studies also suggest a positive correlation between indicators of burnt biomass and fungal presence in particulate matter. In fact, the U.S. Centers for Disease Control and Prevention (CDC) places wildland firefighters at a higher risk for coccidiodomycosis (also known as valley fever), an infection caused by a fungus that is aerosolized during soil disturbance. In October 2020, Moore et al. demonstrated that samples of smoke emitted from controlled burns in regions of North Florida contained 5-fold higher concentrations of microbes compared to ambient air, equivalent to ~7.2 × 109 cells per m2 of burned area. Approximately 80% of these cells were viable, despite their exposure to wildfire temperatures.
The authors also conducted controlled combustion experiments in the laboratory and found a higher abundance of bioaerosols and culturable bacteria emitted from burning dead vegetation compared to fresh shrubs. The authors were able to culture ~6% of microbes and found that many bacteria were associated with taxa commonly found in soil and on plant tissues and root nodules. Both the effect of wildfires on microbial ecology and the study of microbes in wildfire smoke are nascent fields. Most of the studies have been conducted during controlled burns (fires intentionally set by a team of fire experts to restore a healthy ecosystem at a particular place) or during fires generated under lab conditions. Study of naturally occurring wildfires still poses a significant challenge, as their unpredictability makes it difficult to obtain samples prior to ignition, nor can studies be replicated in exactly the same way to generate statistically significant data. The study of microbial composition from different parts of the world with unique climate and soil conditions will be necessary to advance the field of fire ecology and generate predictive models of smoke transport and effects. Such tools will be valuable to mitigate future wildfire challenges posed by changing climate conditions, to restore forests to their healthy states and also to prevent infections caused by fire-generated bioaerosols.”

“By taking a close look at the smoke from prescribed burns, like this 2019 fire among aspen trees in Fishlake National Forest in Utah, researchers have a new view of how wildfires can move living microbes”
PYROAEROBIOLOGY
https://nature.com/articles/s41396-020-00788-8
https://sciencenews.org/article/wildfire-smoke-microbes-air-health-risk-bacteria-fungi
Wildfires launch microbes into the air. How big of a health risk is that?
by Megan Sever / April 13, 2021
“As climate change brings more wildfires to the western United States, a rare fungal infection has also been on the rise. Valley fever is up more than sixfold in Arizona and California from 1998 to 2018, according to the U.S. Centers for Disease Control and Prevention. Valley fever causes coughs, fevers and chest pain and can be deadly. The culprit fungi, members of the genus Coccidioides, thrive in soils in California and the desert Southwest. Firefighters are especially vulnerable to the disease. Wildfires appear to stir up and send the soil-loving fungi into the air, where they can enter people’s lungs. If the fires are helping these disease-causing fungi to get around, could they be sending other microorganisms aloft as well? Leda Kobziar, a fire ecologist at the University of Idaho in Moscow, decided in 2015 to see if she could find out if and how microorganisms like bacteria and fungi are transported by wildfire smoke — and what that might mean for human and ecological health. By 2018, Kobziar had launched a new research field she named “pyroaerobiology.” First, she asked if microorganisms can even survive the searing heat of a wildfire. The answer, she found, is yes. But how far bacteria and fungi can travel on the wind and in what numbers are two of the many big unknowns. With a recent push to spark new collaborations and investigations, Kobziar hopes that scientists will start to understand how important smoke transport of microbes may be.

“For Kobziar’s earliest studies in 2015, her students held up petri dishes on long poles to collect samples of the smoky air near a prescribed fire at the U of Florida experimental forest”
Air may look clear, but even in the cleanest air, “hundreds of different bacteria and fungi are blowing around,” says Noah Fierer, a microbiologist at the University of Colorado Boulder. Winds whisk bacteria and fungi off all kinds of surfaces — farm fields, deserts, lakes, oceans. Those microbes can rise into the atmosphere to travel the world. Scientists have found microorganisms from the Sahara in the Caribbean, for example. Many (if not most) of the airborne microorganisms, including bacteria, fungi and viruses, are not likely to cause disease, Fierer notes. But some can make people sick or cause allergic reactions, he says. Others cause diseases in crops and other plants. The billions of tons of dust that blow off of deserts and agricultural fields each year act as a microbial conveyor belt. In places like Arizona, people know to be alert for symptoms of airborne illnesses like Valley fever after dust storms, since infections increase downwind afterward. If dust can move living microorganisms around the globe, it makes sense that particulates in smoke would be microbe movers too, Kobziar says — assuming the microscopic life-forms can survive a fire and a spin in the atmosphere.
 “Kobziar and colleagues use drones to collect samples at U of Florida experimental forest”
“Kobziar and colleagues use drones to collect samples at U of Florida experimental forest”
Rising temperatures and worsening droughts have led to longer and more intense wildfire seasons across the West (SN: 9/26/20, p. 12). Breathing wildfire smoke makes people sick (SN Online: 9/18/20), even causing premature death from heart and lung illnesses. In the United States, wildfire smoke causes about 17,000 premature deaths per year — a number projected to double by 2100, according to a 2018 study in GeoHealth. In other parts of the world, the effects are far worse. In 2015, smoke from illegal land-clearing blazes plus wildfires in Indonesia killed an estimated 100,000 people across Southeast Asia, according to a 2016 report in Environmental Research Letters. Blame is usually attributed to particulate matter — organic and inorganic particles suspended in the air, including pollen, ash and pollutants. But scientists and health officials are increasingly realizing that there’s an awful lot we don’t know about what else in smoke is affecting human health. The most intense fires, the ones that burn the hottest and release the most energy, can create their own weather systems and send smoke all the way into the stratosphere, which extends about 50 kilometers above Earth’s surface (SN: 9/14/19, p. 12). Once there, smoke can travel around the world just as ash from explosive volcanoes does. Kobziar’s team and others provided compelling evidence in the February ISME Journal that live, viable microorganisms can be carried in smoke plumes — at least near Earth’s surface if not higher up.

“The Fire and Smoke Model Evaluation Experiment, or FASMEE, team set this high-intensity crown fire in the aspens of Fishlake National Forest, Utah, in 2019. The team used a drone to measure microbial concentrations in this smoke.”
In 2015, while at the University of Florida in Gainesville, Kobziar and her students collected the first air samples for this line of research during a series of planned, or prescribed, burns that Kobziar set at the school’s experimental forest. The group arrived at the forest armed with 3-meter-long poles topped with petri dishes to collect samples from the air. Before any fires were set, the team held the petri dishes in the air for three minutes to collect air samples as a pre-fire baseline. Then Kobziar, a certified prescribed burn manager (or as she calls it, a “fire lighter”), lit the fires. Once flames were spreading at a steady rate and smoke was billowing, students hoisted new petri dishes into the smoke, almost as if aiming a marshmallow on a stick at a campfire. This allowed them to collect smoky air samples to compare to the “before” samples. Back in the lab, in a dark room held at a constant 23° Celsius, both the baseline and smoky petri dishes — covered and sealed from further contamination — were left for three days. Microbes began to grow. Far more bacterial and fungal species populated the smoky petri dishes than the baseline dishes, indicating that the fire aerosolized some species that weren’t in the air before the fire, Kobziar says. “We were stunned at how many different microbial colonies survived the combustion environment and grew in the smoke samples, compared to very few in the ambient air,” she says. Based on DNA tests, Kobziar’s team identified 10 types of bacteria and fungi; some are pathogenic to plants, one is an ant parasite and one helps plants absorb nutrients. “This was the moment when the way we thought about smoke was completely transformed,” she says.
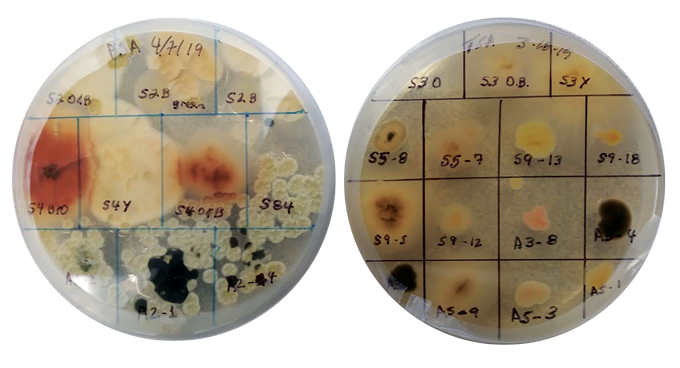
“Petri dishes show bacterial and fungal colonies that grew after five minutes of exposure to smoke from pine needles collected from Florida then burned in Kobziar’s U of Idaho lab”
In 2017, after Kobziar had moved to Idaho, her team collected soil samples from the University of Idaho’s experimental forest and burned them — this time, in the lab. As smoke unfurled above the burning soils, the researchers collected air samples, and again, sealed them and put them in a dark, warm room to see what would grow. After a week, lots of different microbes, including fungi, had multiplied into colonies on the plates, the researchers reported in 2018 in Ecosphere. Since then, Kobziar’s team has collected more air samples during prescribed burns of varying intensities in Florida, Idaho, Montana and Utah, joining forces with the U.S. Forest Service Fire and Smoke Model Evaluation Experiment, or FASMEE, team. For her students’ safety, she’s replaced the poles and petri dishes with drones. She sends a single drone carrying a vacuum pump with a filter into smoke plumes at varying altitudes up to 120 meters, the team described in the journal Fire in 2019.
In every experiment, the researchers have found living bacteria and fungi, many of which were not found in any of the air samples taken before the fires. In Utah smoke samples, for example, the FASMEE team found more than 100 different fungi that were not in the air before the fire, Kobziar says. Findings included species of Aspergillus, which can cause fevers, coughs and chest pain, as well as Cladosporium, molds that can cause allergies and asthma. Whether any of these microorganisms pose a danger to people is unknown, Kobziar cautions. Her team has not tested whether the microbial species that survive the heat can cause disease, but the group plans to do so. The research in Utah revealed another crucial fact: These microbes are tough. Even in smoke from high-intensity, high-temperature fires, about 60 percent of bacterial and fungal cells are alive, Kobziar says. Roughly 80 percent seem to survive lower-intensity fires, which is “about the same percentage of cells we’d expect to see alive in ambient air conditions,” she says. Thus, these first studies show that fires are sending live bacteria and fungi into the air.
“The FASMEE team set up a mobile research lab on the fire line at Fishlake National Forest. Drone operators sent the machines into the smoke to collect samples, back to the “lab” to return samples, then back up to collect more multiple times. They found about 1,000 different microbe types in the smoke.”
And that they can travel at least 120 meters above the ground and close to a kilometer from a flame front. But many basic questions remain, Kobziar says. How do the microbes change — in quantity, type or viability — based on distance traveled away from the flames? How far can they actually go? How do different fuel sources — pine trees, grasslands, deciduous trees or crops, for example — affect microbial release? How does fire intensity affect what is released and how far it travels? Does the type of combustion — smoldering (like a wet log on a campfire) versus high-intensity flaming fires — affect what is released? How does temperature or humidity or weather affect microbial survival? Then, of course, Kobziar has plenty of questions about how to conduct this new field of research: What are the safest and best ways to sample the air in the dangerous environment of an unpredictable wildfire? How do you avoid contaminating the biological samples? She’s been learning as she goes, honing her methodology. The answers to many of those questions could come if one of Kobziar’s dream collaborations comes true: She wants to work with the researchers whose studies involve the NASA DC-8 “flying laboratory,” which explores Earth’s surface and atmosphere for studies ranging from archaeology to volcanology. Researchers have already tracked many different chemicals released by fires into the stratosphere from the Arctic to the South Pacific and everywhere in between, using the DC-8 for NASA’s Atmospheric Tomography Mission, says Christine Wiedinmyer, a fire emissions modeler at the Cooperative Institute for Research in Environmental Sciences in Boulder, Colo. Finding traceable signatures of fires everywhere in the atmosphere suggests that fires could also be sending bacteria and fungi around the world, she says.
“Pyroaerobiology is so cool,” says Wiedinmyer, who tracks and simulates the movement of chemicals in wildfire smoke around the world. She sees no reason that such atmospheric chemistry models couldn’t also be used for tracking and forecasting the movement of microbes in smoke plumes — once researchers collect sufficient measurements. Those data might answer basic questions about the human health hazards of microorganisms in smoke. Microbiologist Fierer in Boulder and Wiedinmyer have collaborated on chemistry sampling and modeling. The two plan to move to bacterial and fungal modeling using data Fierer is gathering on microbial concentrations in wildfire smoke. Kobziar, meanwhile, is working with atmospheric modelers to figure out how to model microbes’ movements in smoke. The long-term aim is to develop models to supplement current air-quality forecasts with warnings of air-quality issues across the United States related to wildfire-released microorganisms in smoke.
While Kobziar’s team focuses on measuring microbes in smoke, Fierer’s team is working to get a baseline of what microbes are in the air at different locations during normal times and then comparing the baseline to smoke. The group has been sampling indoor and outdoor air at hundreds of U.S. homes to “map out what microbes we’re breathing in as we’re walking around doing our daily business,” Fierer says. They are also sampling air across Colorado, which experienced record-breaking fires in 2020 (SN: 12/19/20 & 1/2/21, p. 32). Fierer’s team uses sampling stations with small, high-powered vacuums atop 2-meter-high poles to “sample air for a period of time without smoke. Then boom, smoke hits [the site], we sample for a few days when there’s smoke in the air, and then we also sample afterward,” Fierer says. Analyzing samples from before, during and after a fire is ideal, he says, as there’s tremendous variation in microbial and fungal populations in the air. Near a Midwestern city in winter, for example, microorganisms might include ones associated with local trees or, strangely, dog feces; near a Colorado cattle feedlot in summer, microbes might include those associated with cattle feces.

“Joanne Emerson, then a postdoctoral researcher at the University of Colorado Boulder, samples air atop a 300-meter-tall tower at the Boulder Atmospheric Observatory.”
When the team gets its results — data collection and analysis have been delayed by the pandemic — Fierer says, “we will know the amounts and types of microbes found in wildfire smoke compared with paired smoke-free air samples, and whether those microbes are viable.” At least in Colorado. Once scientists get the measurements of how many microbes can be carried in smoke, and to what altitudes, Fierer’s group can combine that information with global smoke production numbers to come up with “some back-of-the-envelope calculations” of the volume of microbes traveling in smoke plumes. Eventually, he says, scientists could figure out how many are alive, and whether that even matters for human health — still “an outstanding question.” Big leaps forward could be made if more scientists get involved in the research, Fierer and Kobziar both say. This research needs a truly multidisciplinary approach, with microbiologists, forest ecologists and atmospheric scientists collaborating, Fierer says. Going it alone would “be equivalent to a microbiologist studying microbes in the ocean and not knowing anything about oceanography,” he says. Fortunately, after Kobziar and infectious disease physician George Thompson of the University of California, Davis published a call-to-arms paper in Science last December, summing up their pyroaerobiology research and noting key questions, several researchers from different fields expressed interest in investigating the topic. “That’s exactly what we hoped would happen,” Kobziar says.

“Nine kilometers above Earth’s surface, a camera on NASA’s DC-8 flying laboratory took this image of thunderclouds rising above columns of smoke from a fire in eastern Washington on August 8, 2019. Such storms, formed by intense fires, loft particulate matter, chemicals and maybe even microbes into the stratosphere.”
In recent years, Thompson has seen a substantial increase in patients getting Valley fever and other fungal infections after nearby wildfires. He was well aware that when particulate matter in smoke gets into the lungs, it can cause breathing difficulties, pneumonia and even heart attacks. In fact, scientists reported in the Journal of the American Heart Association in April 2020 that exposure to heavy smoke during 2015–2017 wildfires in California raised the risk of heart attacks by up to 70 percent. He began to wonder if California’s record-breaking infernos were stirring up other microbes along with the fungus that causes Valley fever. So he joined forces with Kobziar. The Valley fever link appears to be real, but so far, local. For example, after the 2003 Simi Fire burned through Ventura County, more than 70 people got sick with Valley fever. But whether the Coccidioides fungi can travel to make people sick at a distance from the fire, no one knows. There are ways to figure out if more people, either locally or farther away, are getting sick with bacterial or fungal infections after wildfires. One way, Thompson says, is to look at a community’s antibiotic prescriptions and hospitalizations in the month preceding and the month after a fire: More prescriptions or hospitalizations from bacterial or fungal infections after a fire could indicate a link. In 2019 at the American Transplant Congress meeting, for example, researchers linked California wildfires with increased hospitalizations related to Aspergillus mold and Coccidioides fungi infections. But until we know more about what microbes fires release and where they go, we won’t know how important such a link is for human health, Fierer says. There’s so much we don’t know yet, Thompson agrees. “We still have a lot of work to do. This is sort of the beginning of the beginning of the story.”
PREVIOUSLY
The fire has generated so much heat and energy that it’s created its own weather, with ballooning pyrocumulus clouds that have even created fire tornadoes: https://t.co/dxJOa4KsoU
— San Francisco Chronicle (@sfchronicle) July 21, 2021
PYROCUMULUS CLOUDS
https://spectrevision.net/2021/07/22/pyrocumulus-clouds/
SURVIVING the PYROCENE
https://spectrevision.net/2020/09/11/surviving-the-pyrocene/
CLOUD MICROBIOMES
https://spectrevision.net/2019/10/17/cloud-microbiomes/
